- HOME
- VENUE
- RSVP
- REGISTRY
- CONTACT
- Eyeframe converter files too big
- Lewis capaldi someone you loved free download
- Filemaker pro 10 web publishing
- Chromebook emulator for android
- Rolie polie olie games playhouse disney
- How to make a drop down list in excel 2010
- How to exit tomb raider 2 pc
- Training for genisys 5-0
- Tubedigger bbc iplayer
- Toad diagnostic software srs
- Inazuma eleven go strikers the six stats
- Elgato hd60 obs
- Tamil 80s actress
- Ion discover dj error cant connect
- Modelsim altera full screen
- Brown attention-deficit disorder scales for children
- 40k drop pod doors
- Rocky theme song mix
- Hitman pro trial reset tool download
- F1 2018 monaco
- All about lily chou chou soundtrack download
- Sam broadcaster pro 4-9-8 serial key
- Marumalarchi movie in raj video vision
- Pokemon picross solutions 19 03
- Xojo web browser
- Sniper elite v2


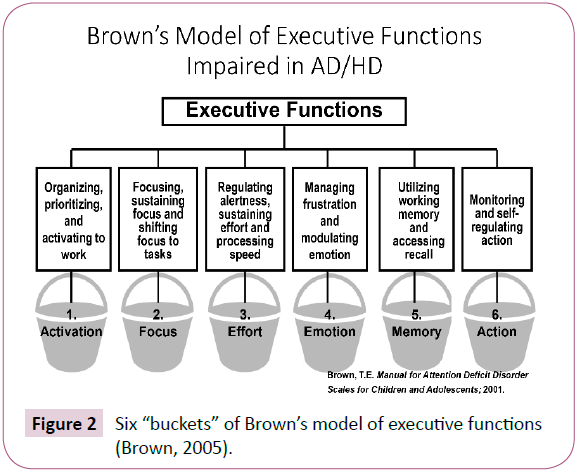
Whereas ADHD is characterized by the typical cognitive and hyperactive/impulsive features of the disorder, bipolar disorder (BPD) is characterized by mood instability, pervasive irritability/rage, grandiosity, psychosis, cyclicity, and lack of response to structure 17. There continues to be much controversy about the validity of the concurrent diagnoses of ADHD and severe mood instability or bipolar disorder. Systematic studies of children and adolescents indicate rates of ADHD ranging from 57% to 98% in bipolar children and conversely, rates of bipolar disorder in 22% of ADHD children and adolescents 16. Interestingly, recent data suggest that stimulant treatment of ADHD over time may decrease the ultimate risk for anxiety and depressive disorders 15.Ī growing literature reports the co-occurrence of bipolar disorder and ADHD. Similarly, ADHD increases the likelihood of having a depressive disorder by at least two-fold 8, 14. High rates of the various anxiety symptoms exist in ADHD and may manifest as social, generalized or panic-like symptoms. In contrast to a disproportionate rate of boys diagnosed with ADHD relative to girls in childhood, in adults, an equal number of men and women with ADHD are presenting for diagnosis and treatment 10.Īnxiety often confounds the diagnosis and treatment of ADHD 3, 11, 12. In more recent years, the recognition and diagnosis of ADHD in adults have been increasing although treatment of adults with ADHD continues to lag substantially behind that of children 8, 9. Across the life span, the social and societal costs of untreated ADHD are considerable, including academic and occupational underachievement, delinquency, motor vehicle safety, and difficulties with personal relationships 3- 5, 6.ĪDHD affects an estimated 4% to 12% of school-aged children worldwide 7 with survey and epidemiologically derived data showing that 4 to 5% of college aged students and adults have ADHD 8. It carries a high rate of comorbid psychiatric problems such as oppositional defiant disorder (ODD), conduct disorder, mood and anxiety disorders, and cigarette and substance use disorders 3. Pharmacotherapy including stimulants, noradrenergic agents, alpha agonists, and antidepressants plays a fundamental role in the long-term management of ADHD across the lifespan.Īttention-deficit/hyperactivity disorder (ADHD) is among the most common neurobehavioral disorders presenting for treatment in children 1, 2. Psychotherapy alone and in combination with medication is helpful for ADHD and comorbid problems. Multimodal treatment includes educational, family, and individual support. Consideration of all aspects of an individual’s life needs to be considered in the diagnosis and treatment of ADHD. The biological underpinning of the disorder is supported by genetic, neuroimaging, neurochemistry and neuropsychological data.
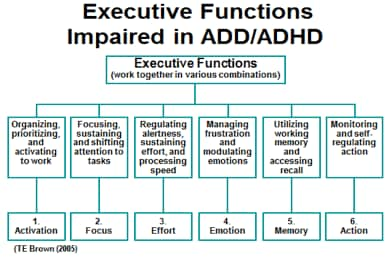
The diagnosis of ADHD is clinically established by review of symptoms and impairment. ADHD is often associated with co-occurring disorders including disruptive, mood, anxiety, and substance abuse. ADHD is often chronic with prominent symptoms and impairment spanning into adulthood. Attention deficit/hyperactivity disorder (ADHD) is among the most common neurobehavioral disorders presenting for treatment in children and adolescents.